Why it is important
Living Liver Donor Questionnaire
Patients with advanced liver disease across the U.S. who are on the liver transplant waiting list face substantial challenges as they need to wait, often for months or years, for a life-saving liver transplant. Unfortunately, with almost 13,000 people on the U.S. liver transplant waiting list, there are simply not enough donated livers from deceased donors, which means that not everyone on the waiting list will survive to receive a life-saving transplant.

Overview of the Living Donor Liver Transplant Procedure
To help solve the deceased donor organ shortage challenge, family members, friends, and even strangers frequently inquire about the option of doing a transplant with a living liver donor.
The transplant team at UWMC is the only group in the Pacific Northwest performing liver transplants in this innovative manner, referred to as Living Donor Liver Transplant (LDLT). Our team performs this surgery in both adults and children who are in need of liver transplant.
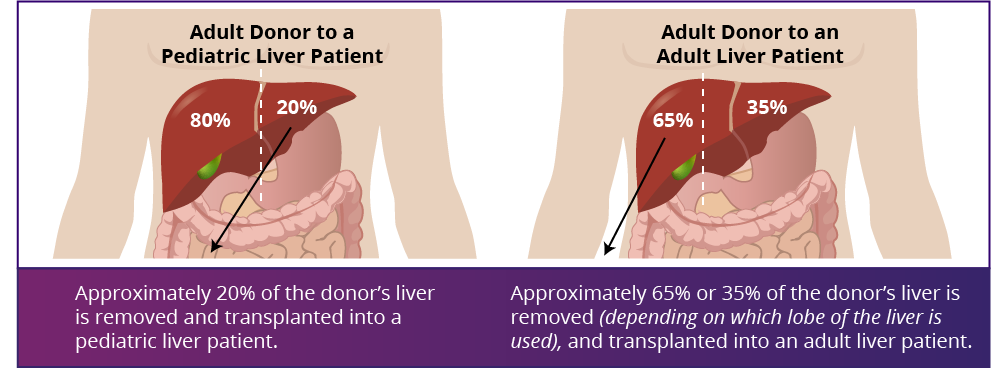
In LDLT, a portion of liver is surgically removed from a healthy living donor and transplanted into the recipient once the diseased liver is removed. LDLT is possible due to the liver’s remarkable ability to regenerate (regrow) in both the liver donor and the recipient. This regeneration is nearly complete by the third month after surgery, with the majority of regeneration being completed within three weeks of surgery. About 50% of living liver donors report a return to their normal life at six weeks and almost all donors are fully recovered after three months from their surgery date.
The ability to perform LDLT and to provide this service to our patients has literally been decades in the making. UWMC and Seattle Children’s Hospital developed the region’s largest experience in deceased donor liver transplantation by performing over 2,000 liver transplants (since 1990) in both adults and children which uses many of the surgical techniques required for LDLT.
We have a dedicated team of liver transplant providers with expertise in LDLT, including: transplant surgeons, hepatologists, transplant nurses, living donor advocates, and social workers. By combining thoughtful and thorough living donor selection with meticulous surgery and dedicated follow up care, our program is committed to providing the absolute best outcomes possible.
For the Recipient
- Significantly shorter time on the national waiting list.
- The ability to be transplanted before one gets critically ill. Your preserved strength at the time of transplant will make your recovery easier and faster.
- The liver from the living donor is of excellent quality.
- The surgery can be scheduled electively, allowing the donor and recipient more time to prepare for surgery.
- The patient survivals are the equal to, or better than, the outcomes experienced in deceased donor transplant.
For the Living Donor
- Life-saving act for your loved one — the vast majority of liver donors share that they would make the same decision to donate after experiencing the entire donation journey.
- Helping a stranger—the gift of transplant that the living donor provides to their intended recipient helps with the overall liver organ scarcity. In this way, being able to transplant one recipient with a living liver donor will ultimately allow another patient on the deceased donor liver waiting list to get a transplant, too.
Living Liver Donation-The Donor's Guidebook
LIVING LIVER DONATION-THE DONOR'S GUIDEBOOK-SPANISH
Living Liver Donor Questionnaire
Volunteering to donate part of your liver with the goal of saving another person’s life is an important decision. Potential donors must initiate the process by contacting the UWMC LDLT team.
The first step for the potential donor is to first learn as much as possible about living donation and what it involves.
To begin the education overview, it is important to understand that a living liver donor:
- Is usually a family member or friend (emotionally related to the intended recipient), but even strangers (non-directed/altruistic) can donate.
- Must be able to understand all of the information regarding liver donation and how to use it to make the best decision.
- Be between the ages of 18 and 60 years.
- Is healthy with no major medical or surgical history.
- Must have a body mass index (BMI) of 32 kg/m2 or less.
- Cannot have significant alcohol intake or abuse illicit drugs.
- Must be free of coercion or external pressure in their decision to donate. In the U.S., the National Organ Transplant Act (NOTA) makes it illegal to buy or sell (receive financial or other gifts or favors) in exchange for human organs.
To help you start thinking about whether living liver donation is the right decision for you, make sure you are a good candidate to be a living liver donor, please ask yourself these questions:
Motives and free will
- Why do I want to donate?
- Is this decision my own? Am I feeling pressured by anyone to be a living liver donor?
- Do I have any unrealistic expectations about being a donor? Am I hoping for a better relationship with the intended recipient? Do I expect publicity, respect, gratitude, or other rewards?
Family and social support
- Will I have enough help from family and friends during my recovery after surgery?
- Do I have a plan for someone who can take care of my children, pets, household, and other duties during my recovery?
- Do my close friends and family understand what is involved with this surgery?
- Do my close friends and family support this donation? If not, what can I do to make sure I get the support I need?
Am I financially able to do this?
- Can I be out of work for 6 weeks to 3 months after my donor surgery?
- Can I handle the hidden costs of being a donor, such as transportation to the hospital and meals away from home?
Handling the pain and stress of major surgery
- Can I handle the physical discomfort of this surgery? This is major surgery. Pain is common with surgery, but usually eases with pain medicines and with time.
- Can I handle the mental and emotional stress of having major surgery?
Recovery from donation surgery
- Will I be able to follow the advice of doctors after surgery? This includes not lifting anything that weighs more than 8 pounds for 2 months.
- Do I have a plan for transport back to the hospital for my follow-up visits?
- Can I commit to a healthy lifestyle after liver donation?
- Can I commit to the follow-up visits I will need after surgery?
Expectations
- Do I have clear and realistic expectations for my own recovery?
- What do I expect for the recipient’s outcome? How would I cope if the liver transplant does not go well?
The idea that one can be a living liver donor or undergo a transplant using a portion of a loved one’s liver may be a completely new idea and concept for many people.
We understand that this donation option may lead to many questions. We are here to provide you with those answers and to supply you with comprehensive educational materials to fully understand the process.
If you are an adult patient at UWMC or if you are the guardian of a pediatric patient at Seattle Children’s Hospital, who is in need of a liver transplant, please contact your pre liver transplant nurse coordinators at either UWMC Liver Transplant Program or Seattle Children’s Hospital to learn more about living donor liver transplantation and how it may be your best option.
In general, any patient who meets criteria to be on the liver transplant waiting list should be considered for LDLT.
Finding a suitable living liver donor is not always easy. A Liver Donor Champion is someone who knows and cares about the liver transplant candidate, who perhaps cannot be a living liver donor himself or herself, but who wants to help the patient. The Liver Donor Champion is willing and eager to learn, and volunteers to serve as an advocate on the patient’s behalf. The UW Medicine Living Liver Donor Team educates the Liver Donor Champion on liver disease, liver transplantation, and provides tips on becoming an effective spokesperson for the liver patient.
The Liver Donor Champion spreads the word about their loved-one’s need for a liver transplant, and about how living liver donation saves lives. Liver Donor Champions reach out to family, friends, and acquaintances to advocate for the liver patient through social media, email, phone, videos, letters, etc.
Learn more about becoming a Donor Champion:
- Living Liver Donor Champion Overview
- Living Liver Donor Champion Overview-SPANISH
- Living Liver Donor Champion Toolkit
Reach out to our Donor Champion team at: liverdonorchampion@uw.edu
If you are interested in, or want to learn more about, becoming a living liver donor: contact our Living Liver Donor Office at 206.598.0337 or by email at liverdonor@uw.edu. Interested donors can also complete our Living Liver Donor Questionnaire.
It is important that the decision to donate be voluntary, so the potential liver donor must initiate the process. No member of the UWMC LDLT transplant team will contact a potential donor initially. Once we get started, our team will provide you with an independent living donor advocate, who will support you from start to finish. Your advocate is available to answer any questions, explain the risks and rewards, and voice any of your concerns to the liver transplant team.